-
Foot Care for Seniors: Maintaining Mobility and Independence
posted: Sep. 20, 2024.

-
How to Manage Foot Pain Caused by Flat Feet
posted: Sep. 10, 2024.
-
The Role of Podiatrists in Sports Medicine and Injury Prevention
posted: Sep. 05, 2024.
-
The Importance of Regular Foot Exams for Diabetics
posted: Aug. 21, 2024.

-
Understanding Diabetic Foot Care
posted: Aug. 07, 2024.
-
Bunion Prevention Tips: How To Avoid the Development or Progression of Bunions
posted: Jul. 12, 2024.

-
The Importance of Proper Footwear
posted: Jul. 10, 2024.

-
Caring for Your Feet as You Age
posted: Jul. 01, 2024.
-
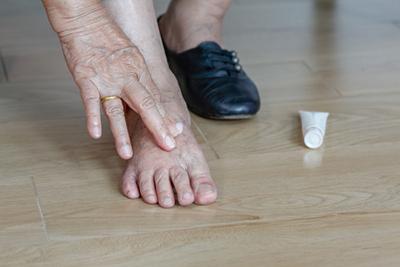
The Benefits of Regular Podiatry Check-Ups
posted: Jun. 13, 2024.
-
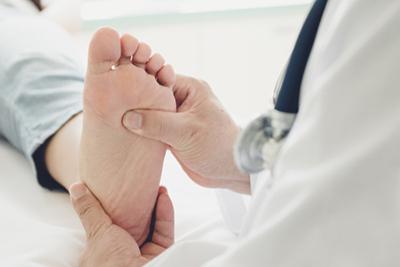
Foot Health Tips for Runners: Preventing Injuries and Maximizing Performance
posted: Jun. 01, 2024.

-
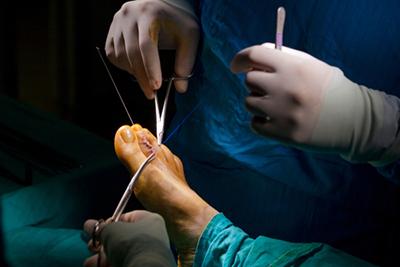
Podiatric Surgery: Procedures for Correcting Foot and Ankle Problems
posted: May 10, 2024.
-
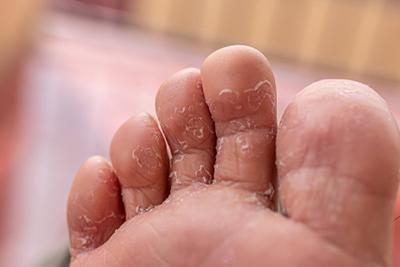
Athlete's Foot: Recognizing and Treating Fungal Infections
posted: May 01, 2024.
-
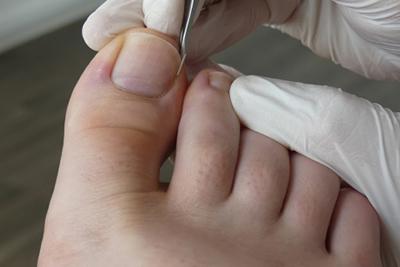
Ingrown Toenails: Causes, Treatment, and Prevention Strategies
posted: Apr. 12, 2024.
-
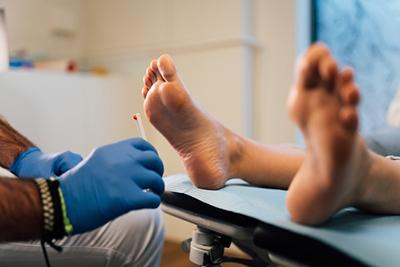
Diabetic Foot Care: Importance, Tips, and Warning Signs
posted: Apr. 07, 2024.
-
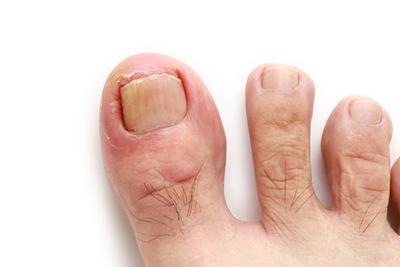
Symptoms of an Ingrown Toenail
posted: Apr. 01, 2024.
-
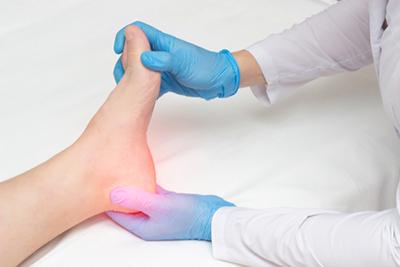
Treating Plantar Fasciitis
posted: Mar. 13, 2024.
3605 Northgate Ct Ste 206
New Albany, IN 47150
(812) 945-9221
(812) 945-7141
Our Location
3605 Northgate Ct Ste 206 New Albany, IN 47150
Hours of Operation
The office is closed from 12:00 to 1:00 for lunch Monday thru Thursday.
Foot First Podiatry
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-4:00 pm
Wednesday:
8:00 am-5:00 pm
Thursday:
8:00 am-5:00 pm
Friday:
8:00 am-1:00 pm
Saturday:
Closed
Sunday:
Closed
